
Written by Astrid Naranjo (Clean Health Accredited Clinical Dietitian)
Before getting into this topic, we are going to start off by saying fat is a macronutrient but depending on the context, fat can also mean different things (e.g. specific molecules, cells, tissue/food, and/or a physical body state). On a cellular level, there are a bunch of different types of fat cells and fat tissue. What most people are referring to when they are talking about the biology of “fat” is white fat cells, especially those located just under the skin (i.e. subcutaneous fat) or as a reserve of energy (1,2).
However, fat serves many more important functions in the human body. Including the following:
– Fat provides a key role for the structure and flexibility of cell membranes and helps to regulate substance movement through the cell membranes.
– Special types of fat (known as eicosanoids) can do specialized hormone signalling, exerting intricate control over many bodily systems, mostly in inflammation or immune function.
– Fat serves the role of an efficient energy store because it can hold a lot of energy per gram. In fact, fat yields more than two times the calories per gram than carbohydrates (9 calories/gram for fat versus 4 calories/gram for carbohydrates). It has been estimated that lean adult men store about 131,000 calories in fat (1).
That is enough energy to sustain life for the average person for approximately 65 days. Excessive fat storage can be unhealthy and/or unwanted. Reducing body fat, whether for health, sports performance or body image reasons, is often a client’s goal when working with a personal trainer or coach, hence let’s get into what the fat burning process means (aka the fat loss physiology).
Fat cells contain beta (burn) and alpha (stubborn) fat receptors, both of which influence fat loss.
In order to lose body fat, fatty acids have to be released from the fat cells into the blood stream. Those fatty acid then need to be transported through the bloodstream to the target tissue where they will be used, and finally they need to be oxidized to create ATP.
So in simple terms, there are 3 phases in the fat burning process:
- Mobilization/Lipolysis
- Transportation
- Oxidization
Mobilization/Lipolysis
Fats, or triglycerides, are made up of three fatty acids and a glycerol backbone. The first step in the fat loss process is to mobilize/get the fat out of the cell (lipolysis), which refers to the release of free fatty acids into the blood steam, so they can be transported. If fatty acids can’t get out of the cell, this will be limiting the whole process, since they won’t be able to be moved/transported to where they need to go to be burned as fuel (3-5).
The first step of the process is controlled by the hormone-sensitive lipase (HSL) which is an intracellular enzyme present in adipose tissue that breaks down stored triglycerides into free fatty acids to then release them into the bloodstream. The HSL is activated primarily by the catecholamines norepinephrine/noradrenaline and epinephrine/adrenaline (stress hormones- the primary players involved in fat mobilization) at the beta fat receptors and generally inhibited by insulin and acylation stimulating protein (ASP) (4).
To ensure the lipolysis can effectively occur, beta receptors need to be stimulated and the alpha receptors inhibited through nutrition, training, and possibly supplementation. This, since the stress hormones are for the most part released through physical stress caused by exercise, a calorie deficit through diet and/or stimulant based supplementation.
As mentioned previously, insulin (a storage hormone- not to be feared!!) can directly inhibit the HSL and thus lipolysis. Insulin is primarily released in response to carbohydrate intake and to lesser degree dietary protein. The ASP which is released in response dietary fat intake is also a potent inhibitor of HSL and thus lipolysis.
Insulin and ASP will both counter the effects of the catecholamines when they are present in the bloodstream. Since these are both controlled by food intake, that is why caloric restriction is important, or fat mobilization will be impaired (1,5-7).
Transportation
Moving to the second phase, fatty acid transportation.
Once fatty acids have been released into the bloodstream, they need to be transported to the place where they will be burned/oxidized as fuel: the muscle or liver cell.
Fatty acid transport is depended on adipose tissue blood flow. If blood flow is good, free fatty acids are bound to albumin and taken to the target area where they will be oxidized. Now, if blood flow is not optimal, fatty acids may get re-esterified or re-stored back into the fat cell.
Some areas like visceral fat have very good blood flow which makes it easier to mobilize and transport fatty acids from those areas (8). Hence, visceral fat tends to move easier than fat in the hips/thighs that have lower blood flow and are higher in alpha receptors (specially in women). This can make it harder for hormones such as the catecholamines to reach those areas (8-10).
Oxidization
The final stage of the fat loss process is oxidation. Fat oxidation refers to the process of breaking down fatty acids.
To oxidize fat one needs:
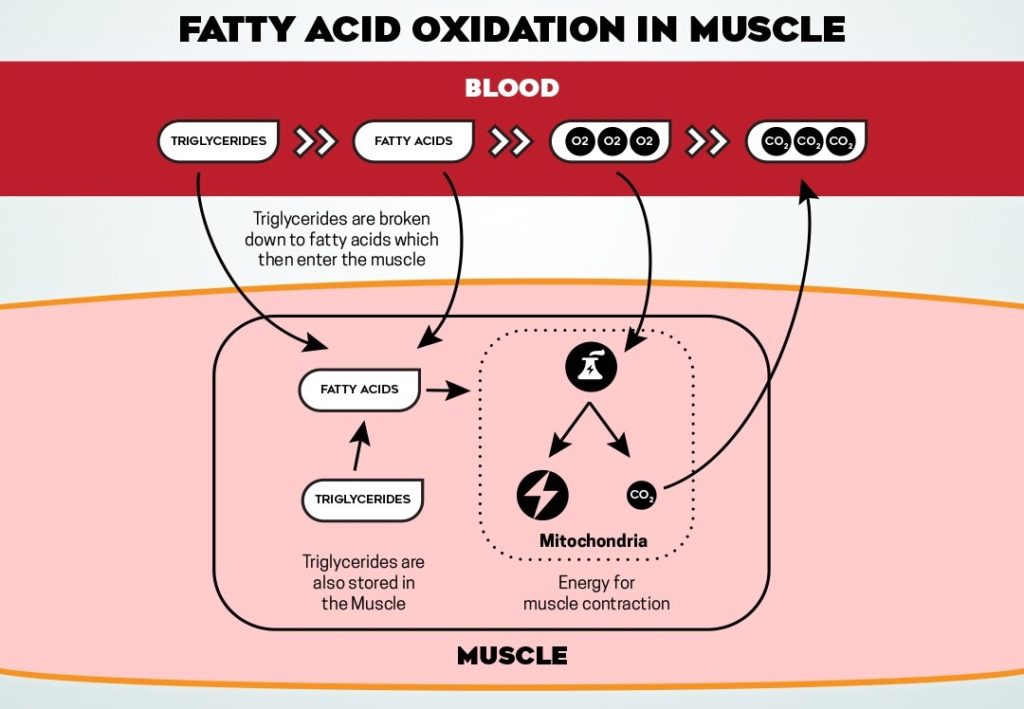
- Healthy mitochondria (small structures in cells that serve as the power plants of the cells. In these power plants, energy is generated for muscle contraction by burning fuel, using oxygen and producing carbon dioxide).
- Supply of fatty acids (these are supplied from triglycerides and fatty acids in the blood, as well as triglycerides stored in the muscle itself)
- Oxygen (transported to the muscle by blood)
If fatty acids are supplied to healthy mitochondria and oxygen is present, fatty acids will be broken down to carbon dioxide. This process is not too dissimilar form burning a log in a fire. You need the fireplace, some wood and oxygen.
Fatty acids need to be transported into the mitochondria by an enzyme called Carnitine palmitoyl-transferase I (CPT1) (11).
CPT1 activity and fat oxidation are primarily regulated by carbohydrate availability, training volume, and dietary fat intake (11,12). When carbohydrate intake is reduced, liver and muscle glycogen become depleted and the body shifts to using preferentially fat for fuel in order to conserve glycogen(12).
A high fat intake in the absence of a caloric deficit, will increase fatty acid oxidation but it will also increase lipogenesis or fat storage (2,12,13). The net effect will be an increase in body fat.
In fact, studies have shown that fat overfeeding increase fat storage more than carbohydrate overfeeding despite increasing fat oxidation (13). That is why a calorie deficit is still required. If you are burning more fat for fuel but also storing more fat it won’t do very much.
Remember, fat oxidation and fat loss are not synonymous.
So then, why are we so obsessed with fat burning?
In order to lose fat we need to be in negative energy balance. In other words: you need to burn more calories than you ingest (and this is superior to exercise and even more to supplements). If you burn more fat through exercise or utilizing stimulant based supplements but you eat more calories than the calories you burn in total, you will not lose fat. Of course, when you are in negative energy balance, you want to make sure that the weight you are losing is mostly fat and this is where fat burning becomes more important (2,4).
The take home message here is: For fat loss negative energy balance is far more important than fat oxidation per se. Fat oxidation and fat loss are not synonymous.
If you would like to learn more about how to design specific diets for clients from all walks of life to maximize results for fat loss, click here to enrol into the Performance Nutrition Coach Collection!
References
- Horowitz, J.F, and Klein, S. (2000.) Lipid metabolism and endurance exercise. American Journal of Clinical Nutrition. 72 (suppl), 558S-563S.
- Venables MC1, Achten J, Jeukendrup AE. Determinants of fat oxidation during exercise in healthy men and women: a cross-sectional study. J Appl Physiol 2005 Jan;98(1):160-7.
- Achten, J., & Jeukendrup, A.E. (2012). Optimizing fat oxidation through exercise. Nutrition. 20, 7-8.
- Duncan, R.E, Ahmadian, M., Jaworski, K., Sarkadi-Nagy, E., & Sul, H.S. (2007). Regulation of lipolysis in adipocytes. Annual Review of Nutrition. 27, 79-101
- Holloway, G.P., Luiken, J.J.F.P., Glatz, J.F.C., Spriet, L.L., & Bonen, A. (2008). Contribution of FAT/CD36 to the regulation of skeletal muscle Fatty acid oxidation: an overview. Acta Physiologica, 192, 293-309.
- Jamurtas, A.Z, Koutedkis, Y., Paschalis, V., Tafa, T, Yfanti, C., Tsiokanos, A, Koukoulis, G., et al. (2004). The effect of a single bout of exercise on resting energy expenditure and respiratory exchange ratio. European Journal of Applied Physiology. 92: 393-398.
- Robergs RA, Ghiasvand F, and Parker D. (2004). Biochemisty of exercise-induced metabolic acidosis. American Journal of Physiology – Regulatory, Integrative and Comparative Physiology. 287 (3), 502-516.
- Antti PM, et al. Effects of weight loss on visceral and abdominal subcutaneous adipose tissue blood-flow and insulin-mediated glucose uptake in healthy obese subjects, Annals of Medicine. 2009;41:2, 152-160, DOI: 10.1080/07853890802446754
- Millet L, Barbe P, Lafontan M, Berlan M, Galitzky J. Catecholamine effects on lipolysis and blood flow in human abdominal and femoral adipose tissue. J Appl Physiol 1998; 85: 181–188.
- Tan G, Goossens GH, Humphreys SM, Vidal H, Karpe F. Upper and lower body adipose tissue function: a direct comparison of fat mobilization in humans. Obes Res 2004; 12: 114–118
- Goedecke JH, Gibson ASC, Grobler L, Collins M, Noakes TD, Lambert EV: Determinants of the variability in respiratory exchange ratio at rest and during exercise in trained athletes. American Journal of Physiology – Endocrinology and Metabolism. 2000; 279: E1325-E1334.
- Essen-Gustavsson B & Tesch PA. Glycogen and triglyceride utilization in relation to muscle metabolic characteristics in men performing heavy-resistance exercise. European Journal of Applied Physiology. 1990;61, 5-10
- Horton TJ, et al. Fat and carbohydrate overfeeding in humans: different effects on energy storage. American Journal of Clinical Nutrition. 1995; 62(1):19-29.






