
Written by Astrid Naranjo (Clean Health Accredited Clinical Dietitian)
Inflammation has gained much attention as a threat to human health, owing to its association with such debilitating and sometimes life-threatening chronic conditions as Alzheimer’s disease, cardiovascular disease, and rheumatoid arthritis (1,5-6).
Nevertheless, despite being increasingly perceived as a harmful process, inflammation is a function essential to life and it is not always is the devil of the story.
Without inflammatory processes to engage the immune system, to help destroy invading organisms, promote clotting and complement activation, and initiate repair mechanisms, our survival as humans would be potentially at risk (7-10).
Considering inflammation as a causative agent in aging or disease goes against the underlying mechanisms whereby the acute inflammatory response is necessary for survival (7,8).
Chronic inflammation inevitably has initiating mechanisms that include immune, autoimmune, and metabolic pathways, leading to the activation and presence of the host-protective response. In this sense, it would be more appropriate to understand and to target the underlying initiating conditions & triggers than the actual inflammatory process that ensues and treat the basic mechanisms of disease rather than interfere in a very important protective mechanism of the host (7-9,11).
Before we dive further into this topic, click here to enrol into our Performance Nutrition Coach Collection and SAVE with our Black Friday Sale! You will learn an advanced, scientific insight into nutrition and key interactions in physiology & how these ultimately impact overall health and results.
So, when you think about inflammation, what crosses through your mind? Do you understand what inflammation is?
There are generally two types of inflammation: acute and chronic (1-3,5).
Acute inflammation, on the one hand, refers to the rapid response of our body to tissue damage due to trauma, microbial invasion, or noxious compounds. Acute inflammation can become severe in a short time and symptoms may last for a few days for example cellulitis or acute pneumonia until the problem is solved or fought (1,2).
Chronic inflammation, on the other hand, refers to as slow, long-term inflammation lasting for prolonged periods of time (from several months to years) (1-3).
It is usually a result of single or multiple factors that impact our body’s homeostasis (12) such as:
- Failure of eliminating the agent causing an acute inflammation
- Exposure to a low level of a particular irritant or foreign material
- An autoimmune disorder
- A defect in the cells responsible for mediating inflammation leading to persistent or recurrent inflammation
- Recurrent episodes of acute inflammation (i.e tuberculosis and rheumatoid arthritis)
- Inflammatory and biochemical inducers that cause oxidative stress and mitochondrial dysfunction
- Chronic stress improperly managed
Chronic inflammation is an essential component of chronic diseases. Additionally, evidence suggests that excessive inflammation may play a critical role in the pathophysiology of the stress-related diseases, yet the basis for this connection is not fully understood (12).
Accumulating researches suggested that excessive inflammation plays critical roles in relationship between stress and stress-related diseases(12). Chronic inflammatory diseases are amongst the most significant cause of deaths in the world which includes type 2 diabetes, metabolic diseases (12,15-16), arthritis and joint diseases, allergies, depression (18), atherosclerosis, non-alcoholic fatty liver disease (NAFLD) (17) , Alzheimer’s disease (19), cancer (20,21) and chronic obstructive pulmonary disease (COPD) (1,4,12).
Amongst many risk factors for chronic inflammation such as age, obesity, diet, smoking, low sex hormones, sleep disorders and chronic stress (1), the later seems to have an important correlation to in the activation of inflammatory responses in the brain as well as peripherally (12-14).
Several risk factors promote a low-level inflammatory response. These include:
Age:
Increasing age is positively correlated with elevated levels of several inflammatory molecules. The age-associated increase in inflammatory molecules may be due to mitochondrial dysfunction or free radical accumulation over time and other age-related factors like an increase in visceral body fat.
Obesity:
Many studies have reported that fat tissue is an endocrine organ, secreting multiple adipokines and other inflammatory mediators. Some reports show that the body mass index of an individual is proportional to the amount of pro-inflammatory cytokines secreted. Metabolic syndrome typifies this well.
Diet:
Diet rich in saturated fat, trans-fats, or refined sugar is associated with higher production of pro-inflammatory molecules, especially in individuals with diabetes or overweight individuals.
Smoking:
Cigarette smoking is associated with lowering the production of anti-inflammatory molecules and inducing inflammation.
Low Sex Hormones:
Studies show that sex hormones like testosterone and estrogen can suppress the production and secretion of several pro-inflammatory markers and it has been observed that maintaining sex hormone levels reduces the risk of several inflammatory diseases.
Stress and Sleep Disorders:
Both physical and emotional stress is associated with inflammatory cytokine release. Stress can also cause sleep disorders. Since individuals with irregular sleep schedules are more likely to have chronic inflammation than consistent sleepers, sleep disorders are also considered as one of the independent risk factors for chronic inflammation.
Common signs and symptoms of chronic inflammation include (1,3,5-6):
- Body pain
- Constant fatigue and insomnia
- Depression, anxiety and mood disorders
- Gastrointestinal complications like constipation, diarrhea, and acid reflux
- Weight gain
- Frequent infections
Two blood tests which are inexpensive and good markers of systemic inflammation include high-sensitivity C-reactive protein (hsCRP) and fibrinogen. High levels of hs-CRP indicate inflammation, but not specifically chronic inflammation since levels are also elevated in acute inflammation resulting from a recent injury or sickness (10).
Many dietary and lifestyle changes may be helpful in reducing chronic inflammation including:
1. Increase intake of nutritious foods with anti-inflammatory properties/compounds
It is important to reduce the consumption of simple added sugars, extra refined carbohydrates, high-glycaemic foods, trans and saturated fats, and hydrogenated oils. Consuming whole grains, natural foods, plenty of vegetables and fruits such as avocados, cherries, kale, and fatty fish like salmon is helpful in reducing inflammation (1,2,25).
2. Lose body fat
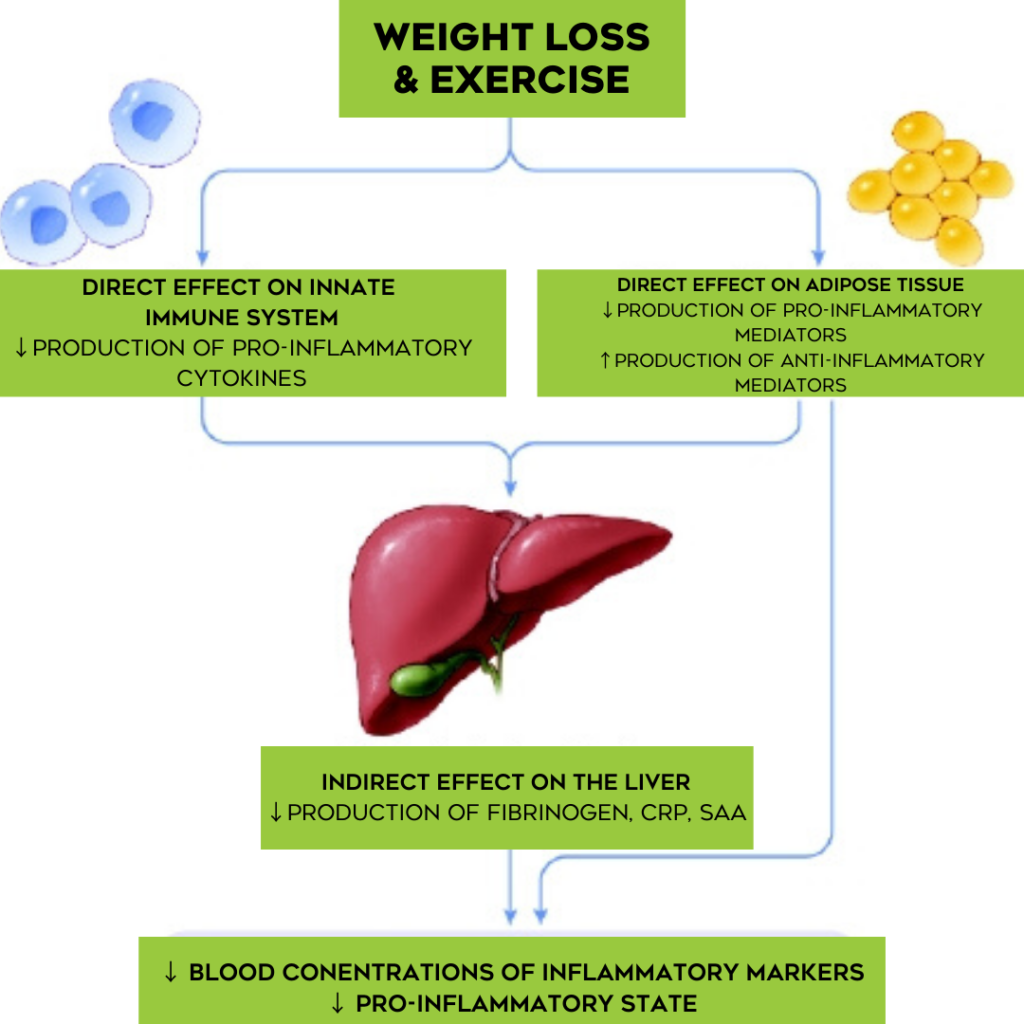
Adipocytes and adipose tissue infiltration with inflammatory cells, are an important source of adipokines production, and their expansion due to overnutrition is responsible for increased in inflammation. The reduction of body fat following both controlled diets or gastric surgery can be favourable in the reduction of pro-inflammatory cytokines (1,22,25). In obese and overweight subjects weight loss, induced both by energy-restricted diet or surgery, is a determinant factor for reducing the level of pro-inflammatory markers.
Hypocaloric diet has an anti-inflammatory effect independent of the diet composition which can play an important role in the prevention of chronic diseases (22,25).
3. Exercise & move regularly
It is well known that adipose tissue in obese or overweight individuals induces low-grade systemic inflammation. Regular exercise helps not only in controlling weight but has also been shown to lowers multiple pro-inflammatory molecules and cytokines independently of weight loss (4,6,23). Large population-based cohort studies consistently show an inverse association between markers of systemic inflammation and physical activity or fitness status, and data from several small-scale intervention studies support that exercise training diminishes inflammation (24,25).
4. Improve sleep quality and quantity
Overnight sleep, ideally at least 7 to 8 hours, stimulates human growth hormone and testosterone which aids the body to repair and rebuild itself (3).
5. Find ways to manage and reduce stress
Chronic psychological stress is linked to greater risk of depression, heart disease, and the body losing its ability to regulate the inflammatory response and normal defence. Meditation and yoga have been shown to be helpful in alleviating stress-induced inflammation and its harmful effects on the body (5-8).
Hopefully now you can appreciate the massive impact stress has on all the systems of the body, you have a better understanding of the negative effects of stress, and you are equipped with some tools on how to better manage stress through diet and lifestyle.
References
- Pahwa R, Goyal A, Bansal P, et al. Chronic Inflammation. [Updated 2020 Aug 10]. In: StatPearls [Internet]. Treasure Island (FL): StatPearls Publishing; 2020 Jan-. Available from: https://www.ncbi.nlm.nih.gov/books/NBK493173/
- Michels da Silva D, Langer H, Graf T. Inflammatory and Molecular Pathways in Heart Failure-Ischemia, HFpEF and Transthyretin Cardiac Amyloidosis. Int J Mol Sci. 2019 May 10;20(9)
- Hang X, Wu X, Hu Q, Wu J, Wang G, Hong Z, Ren J., Lab for Trauma and Surgical Infections. Mitochondrial DNA in liver inflammation and oxidative stress. Life Sci. 2019 Nov 01;236:116464
- Sharma H. Meditation: Process and effects. Ayu. 2015;36(3):233–237. doi:10.4103/0974-8520.182756
- Gauldie J. Inflammation and the aging process: devil or angel. Nutr Rev. 2007 Dec;65(12 Pt 2):S167-9. doi: 10.1111/j.1753-4887.2007.tb00356.x. PMID: 18240542.
- McGeer EG, Klegeris A, McGeer PL. Inflammation, the complement system and the diseases of aging. Neurobiol Aging. 26(suppl):94 –97.
- Baumann H, Gauldie J. The acute phase response. Immunol Today. 1994;15:74 – 80.
- Gauldie J, Richards C, Baumann H. IL6 and the acute phase reaction. Res Immunol. 1992;143:755–759.
- Allison AC, Ferluga J, Prydz H, Schorlemmer HU. The role of macrophage activation in chronic inflammation. Agents Actions. 1978;8:27–35.
- Blackman MA, Yates JL, Spencer CM, Vomhof-DeKrey EE, Cooper AM, Leadbetter EA. The Yin and Yang of inflammation. Curr Mol Med. 2014;14(9):1238-43. doi: 10.2174/1566524014666141015161344. PMID: 25323997; PMCID: PMC4311872.
- Neves J, Sousa-Victor P. Regulation of inflammation as an anti-aging intervention. FEBS J. 2020 Jan;287(1):43-52. doi: 10.1111/febs.15061. Epub 2019 Oct 9. PMID: 31529582.
- Liu, Y. Z., Wang, Y. X., & Jiang, C. L. (2017). Inflammation: The Common Pathway of Stress-Related Diseases. Frontiers in human neuroscience, 11, 316. https://doi.org/10.3389/fnhum.2017.00316
- Rohleder N. Stimulation of systemic low-grade inflammation by psychosocial stress. Psychosom Med. 2014 Apr;76(3):181-9. doi: 10.1097/PSY.0000000000000049. PMID: 24608036.
- Calcia MA, Bonsall DR, Bloomfield PS, Selvaraj S, Barichello T, Howes OD. Stress and neuroinflammation: a systematic review of the effects of stress on microglia and the implications for mental illness. Psychopharmacology (Berl). 2016 May;233(9):1637-50. doi: 10.1007/s00213-016-4218-9. Epub 2016 Feb 5. PMID: 26847047; PMCID: PMC4828495.
- Kuo LE, Czarnecka M, Kitlinska JB, Tilan JU, Kvetnanský R, Zukowska Z. Chronic stress, combined with a high-fat/high-sugar diet, shifts sympathetic signaling toward neuropeptide Y and leads to obesity and the metabolic syndrome. Ann N Y Acad Sci. 2008 Dec;1148:232-7. doi: 10.1196/annals.1410.035. PMID: 19120115; PMCID: PMC2914537.
- Tsuneki H, Tokai E, Sugawara C, Wada T, Sakurai T, Sasaoka T. Hypothalamic orexin prevents hepatic insulin resistance induced by social defeat stress in mice. Neuropeptides. 2013 Jun;47(3):213-9. doi: 10.1016/j.npep.2013.02.002. Epub 2013 Mar 16. PMID: 23510906.
- Ma KL, Ruan XZ, Powis SH, Chen Y, Moorhead JF, Varghese Z. Inflammatory stress exacerbates lipid accumulation in hepatic cells and fatty livers of apolipoprotein E knockout mice. Hepatology. 2008 Sep;48(3):770-81. doi: 10.1002/hep.22423. PMID: 18752326.
- Norman GJ, Karelina K, Zhang N, Walton JC, Morris JS, Devries AC. Stress and IL-1beta contribute to the development of depressive-like behavior following peripheral nerve injury. Mol Psychiatry. 2010 Apr;15(4):404-14. doi: 10.1038/mp.2009.91. Epub 2009 Sep 22. PMID: 19773812; PMCID: PMC5214062.
- Chen CH, Zhou W, Liu S, Deng Y, Cai F, Tone M, Tone Y, Tong Y, Song W. Increased NF-κB signalling up-regulates BACE1 expression and its therapeutic potential in Alzheimer’s disease. Int J Neuropsychopharmacol. 2012 Feb;15(1):77-90. doi: 10.1017/S1461145711000149. Epub 2011 Feb 18. PMID: 21329555.
- Krizanova O, Babula P, Pacak K. Stress, catecholaminergic system and cancer. Stress. 2016 Jul;19(4):419-28. doi: 10.1080/10253890.2016.1203415. Epub 2016 Jul 11. PMID: 27398826.
- Thaker PH, Han LY, Kamat AA, Arevalo JM, Takahashi R, Lu C, Jennings NB, Armaiz-Pena G, Bankson JA, Ravoori M, Merritt WM, Lin YG, Mangala LS, Kim TJ, Coleman RL, Landen CN, Li Y, Felix E, Sanguino AM, Newman RA, Lloyd M, Gershenson DM, Kundra V, Lopez-Berestein G, Lutgendorf SK, Cole SW, Sood AK. Chronic stress promotes tumor growth and angiogenesis in a mouse model of ovarian carcinoma. Nat Med. 2006 Aug;12(8):939-44. doi: 10.1038/nm1447. Epub 2006 Jul 23. PMID: 16862152.
- Adipocytes and adipose tissue infiltration with inflammatory cells, are an important source of adipokines production, and their expansion due to overnutrition is responsible for increased in inflammation. The reduction of body fat following both controlled diets or gastric surgery can be favorable in the reduction of pro-inflammatory cytokines.
- Nicklas, Barbara J, and Tina E Brinkley. “Exercise training as a treatment for chronic inflammation in the elderly.” Exercise and sport sciences reviews vol. 37,4 (2009): 165-70. doi:10.1097/JES.0b013e3181b7b3d9
- Beavers, Kristen M et al. “Effect of exercise training on chronic inflammation.” Clinica chimica acta; international journal of clinical chemistry vol. 411,11-12 (2010): 785-93. doi:10.1016/j.cca.2010.02.069
- Nicklas BJ, You T, Pahor M. Behavioural treatments for chronic systemic inflammation: effects of dietary weight loss and exercise training. CMAJ. 2005 Apr 26;172(9):1199-209. doi: 10.1503/cmaj.1040769. PMID: 15851714; PMCID: PMC557073.






